You clean your teeth carefully. You use a decent toothbrush, you rinse regularly, and yet there it is – that warm, golden, slightly dull tone that no amount of effort seems to shift. A brasssmile is one of those things that creeps up quietly. Most people do not notice it developing until a photograph catches them off guard, or until they compare their smile to someone else’s in a well-lit room and realise the difference is more than just lighting.
The frustrating part is that a brasssmile is rarely caused by one thing. It builds over time through the combined effects of what you eat and drink, how your body is ageing, the specific chemistry of your own enamel, and sometimes factors completely outside your control — like the medication you were prescribed years ago. Understanding each cause is not just useful knowledge. It is the foundation of any genuinely effective solution. You cannot treat what you have not correctly identified.
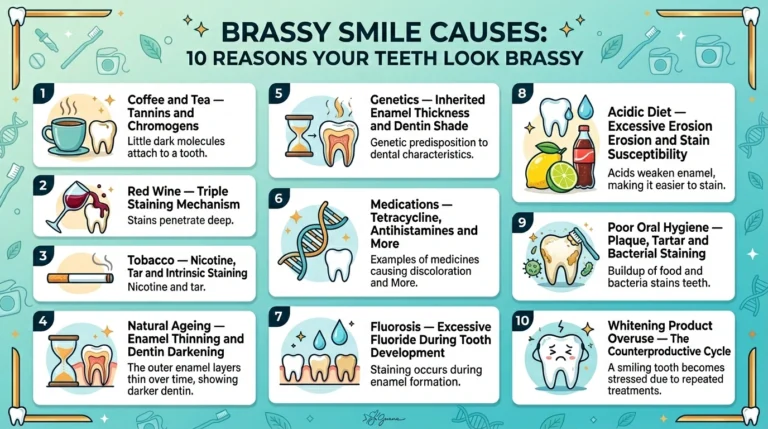
This guide breaks down the 10 most established and well-documented causes of brasssmile, drawing on dental science, clinical observations, and real-world experience. Each section is designed to help you recognise whether a particular cause applies to you — so that when you reach for a solution, you are reaching for the right one.
Understanding the Anatomy Behind Brasssmile: Enamel, Dentin and Colour
▶ Brasssmile develops primarily because tooth enamel — the outer protective layer — becomes thinner or more stained over time, allowing the naturally yellow dentin beneath to show through. The combination of surface pigmentation and exposed dentin creates the warm, brassy tone that defines this condition. Understanding this mechanism is essential to identifying which cause applies to you.
Before exploring the individual causes of brasssmile, it helps to understand the structural reason teeth develop a brassy appearance at all. Human teeth are composed of multiple layers. The outermost layer, enamel, is a semi-translucent mineralised tissue — the hardest biological substance in the human body. Beneath it sits dentin, a porous calcified material that is inherently yellow in colour. The whiter and thicker your enamel, the more it masks that underlying yellow. As enamel thins or picks up surface pigmentation, dentin becomes visible — and the result is the warm, brassier tone familiar to anyone dealing with this condition.
Enamel does not regenerate once it is lost. This makes the causes of enamel thinning particularly significant — because the damage accumulates silently and the visual consequences often only become apparent years after the underlying process began. Equally, surface staining can penetrate the enamel pellicle — a thin protein film that naturally coats teeth — and settle into micro-pores in the enamel surface, where brushing alone cannot reach it. Both of these mechanisms are at work in most brasssmile cases, and most of the causes below contribute to one or both of them.
💡 Enamel lost through acid erosion or abrasion cannot grow back. This is why preventing the causes of enamel thinning matters as much — if not more — than treating existing discolouration.
The 10 Proven Causes of Brasssmile: A Complete Breakdown
▶ The 10 established causes of brasssmile are: daily coffee and tea consumption, red wine and dark-pigmented drinks, tobacco and smoking, natural ageing and enamel wear, genetic enamel composition, certain prescription medications, fluorosis from excessive fluoride exposure, acidic diet and enamel erosion, poor or inconsistent oral hygiene habits, and overuse or misuse of whitening products. Most brasssmile cases involve two or more of these simultaneously.
☕ Cause 1: Coffee and Tea: Tannins That Penetrate Enamel
Coffee and tea are the most widely consumed hot beverages in the world — and they are also among the most consistent contributors to brasssmile. The mechanism is specific and well understood. Both beverages are rich in tannins, a class of polyphenolic compounds found naturally in plants. Tannins have an unusual molecular property: they bind readily to proteins, including the salivary proteins that form the enamel pellicle on your teeth.
Once tannins bind to this pellicle, they create a sticky chromogen-trapping layer that accumulates with each cup consumed. The chromogens — intensely pigmented molecules also present in both coffee and tea — embed into this tannin-pellicle complex and resist removal by ordinary brushing. Tea is often more damaging than coffee in this regard because black and green teas typically contain a higher concentration of tannins per serving. Darker roasts of coffee present a higher chromogen load. The combination of frequency, contact time, and incomplete rinsing is what converts a daily pleasure into a long-term contributor to brasssmile.
🍷 Cause 2: Red Wine: The Triple Staining Mechanism
Red wine represents one of the most chemically aggressive contributors to brasssmile because it operates through three distinct mechanisms simultaneously. First, like tea and coffee, it is rich in tannins that bind to enamel pellicle and trap chromogens. Second, red wine is significantly acidic — with a pH typically between 3.0 and 3.5 — low enough to temporarily soften enamel through a process called acid erosion. Softened enamel is more porous and absorbs staining compounds more readily.
Third, red wine contains its own deeply pigmented chromogens derived from grape skin anthocyanins. These molecules are responsible for wine’s characteristic colour and are highly reactive with tooth enamel surfaces. The practical result is that drinking red wine without rinsing afterward creates a window in which acidified, softened enamel is directly exposed to large concentrations of binding tannins and vivid chromogens — an ideal set of conditions for accelerating brasssmile. White wine, while less pigmented, contributes to brasssmile through its high acidity alone.
🚬 Cause 3: Tobacco: Nicotine, Tar and Deep Intrinsic Staining
Tobacco products cause tooth discolouration through a more serious mechanism than most dietary factors — one that involves intrinsic as well as extrinsic staining. Nicotine, in its base form, is colourless. However, it oxidises readily on contact with oxygen and turns a characteristic yellow-brown pigment. This oxidised nicotine penetrates enamel pores and embeds within the enamel matrix itself, making it resistant to standard surface whitening approaches.
Tar, the second major staining agent in tobacco smoke, is inherently dark and sticky. It adheres to tooth surfaces and to existing deposits of plaque and tartar, creating increasingly thick layers of discolouration with each exposure. Smokeless tobacco products — including chewing tobacco and snus — produce similar intrinsic staining, often concentrated near the gumline where prolonged contact occurs. Tobacco-related brasssmile is among the most resistant to home treatment because it involves genuinely intrinsic pigmentation that peroxide-based strips and pastes may only partially address.
⏳ Cause 4: Natural Ageing: The Inevitable Enamel Thinning
Ageing is the one cause of brasssmile that applies universally, regardless of lifestyle, diet, or oral hygiene discipline. Over the course of a lifetime, enamel gradually wears down through the cumulative effect of daily use — chewing, brushing, and exposure to even mildly acidic foods and drinks. This process, known as physiological attrition and erosion, is slow enough that most people do not notice it happening, but the visual consequences become apparent from the thirties onward for many individuals.
Simultaneously, the dentin beneath the enamel undergoes its own age-related changes. Secondary dentin — laid down by the tooth’s living pulp in response to stimuli over time — gradually narrows the pulp chamber and increases the density and yellowing of dentin tissue. The combined effect of thinning translucent enamel above and darkening dentin below creates a steadily worsening brasssmile that no amount of surface whitening can permanently counteract. This is the most purely structural form of brasssmile, and it is one reason why professional treatments like veneers become increasingly relevant as patients move into their forties and fifties.
🧬 Cause 5: Genetics: Inherited Enamel Thickness and Dentin Colour
Genetic variation plays a more significant role in brasssmile than many people realise. The natural thickness of tooth enamel and the inherent shade of the underlying dentin are both substantially heritable traits. Some individuals are born with naturally thinner enamel — a condition sometimes described as enamel hypoplasia in its clinical form — meaning their dentin colour is more visible from the outset, independent of any lifestyle or dietary factors.
Dentin shade itself also varies genetically. In some individuals it is closer to pale yellow; in others, it is a richer, darker yellow-brown tone. The shade of your natural dentin sets the floor of what whitening can achieve — because whitening can lighten surface staining and even penetrate enamel to bleach chromogens within it, but it cannot change the fundamental colour of dentin below a certain depth. If your parents or siblings have always had a notably warm or brassy smile despite good oral hygiene practices, genetics is likely a contributing factor in your own case. This should shape your expectations of home whitening and point you toward professional options that address colour structurally.
💊 Cause 6: Medications: Tetracycline, Antihistamines and More
Several categories of prescription medication are clinically documented causes of tooth discolouration, and in many cases this discolouration contributes directly to brasssmile. The most extensively studied example is the tetracycline family of antibiotics. When tetracycline is taken during childhood — specifically during the years when permanent teeth are mineralising, typically from before birth to around age eight — the antibiotic molecules incorporate into the developing dentin and enamel, producing a characteristic grey-yellow banding or generalised warmth that persists into adulthood.
Beyond tetracyclines, other medications associated with tooth discolouration include certain antihistamines (including chlorhexidine-containing mouthwashes used long-term, which can produce brown surface staining), some blood pressure medications, antipsychotic medications including certain phenothiazines, and chemotherapy agents. Iron supplements taken in liquid form can produce green-brown surface staining. Many of these effects are dose-dependent and long-term in nature, meaning the discolouration is often only noticed years after the medication was taken — making the causal link easy to miss.
💧 Cause 7: Fluorosis: When Protective Fluoride Becomes Excessive
Fluoride is one of the most important tools in preventive dentistry — it remineralises enamel, reduces cavity risk, and strengthens developing teeth. However, excessive fluoride exposure during the years when adult teeth are forming can disrupt normal enamel mineralisation, resulting in a condition known as dental fluorosis. Mild fluorosis presents as white flecks or streaks on the enamel surface. Moderate to severe cases produce brown or yellow-brown spots, patches, and pitting that contribute to a visible brasssmile.
Fluorosis is primarily a concern in areas where drinking water contains naturally elevated fluoride concentrations, in children who swallow toothpaste regularly during early childhood, or in those who take fluoride supplements in addition to existing dietary fluoride sources. It is worth noting that once fluorosis marks have formed, they are permanent structural features of the enamel — they cannot be removed by whitening, though their visual impact can be reduced through professional microabrasion, bonding, or veneers. The prevalence of mild fluorosis is higher than most people expect, making it a more common contributor to brasssmile than it is typically given credit for.
🍋 Cause 8: Acidic Diet: Enamel Erosion and Increased Stain Susceptibility
Dietary acid is one of the most insidious contributors to brasssmile because its effects are both cumulative and invisible until significant damage has occurred. Foods and drinks with a pH below 5.5 — the approximate threshold at which enamel begins to dissolve — include citrus fruits and juices, carbonated drinks (including sparkling water), vinegar-based dressings, fermented foods, wine, and many sports and energy drinks. Regular exposure to these acidic substances progressively softens and removes enamel through a chemical process called acid erosion.
Eroded enamel is thinner, more translucent, and more porous — all characteristics that make brasssmile worse. Thinner enamel allows more dentin colour to show through. More porous enamel absorbs chromogens from food and drink more readily. In practice, someone whose diet is chronically high in acidic foods will experience faster progression of brasssmile than someone with a neutral-pH diet, even if every other factor is identical. The combination of a high-acid diet with regular coffee, tea, or wine consumption compounds this effect significantly.
🪥 Cause 9: Poor Oral Hygiene: Plaque, Tartar and Bacterial Staining
While brasssmile is certainly not exclusively a hygiene problem — many highly diligent brushers still develop it — poor or inconsistent oral hygiene can significantly accelerate and worsen tooth discolouration. Dental plaque is a biofilm of bacteria that continuously forms on tooth surfaces. When not removed regularly through brushing and interdental cleaning, it thickens and calcifies into tartar, also known as dental calculus. Both plaque and tartar are yellow-to-brown in colour and adhere to tooth surfaces in ways that make them impossible to remove without professional intervention.
Beyond the direct visual contribution of plaque and tartar, the bacterial activity within plaque produces acids that contribute to enamel erosion, and the metabolic by-products of certain oral bacteria include chromogenic compounds that add additional pigment to tooth surfaces. Irregular brushing technique — for example, missing the gumline consistently — leads to discolouration that concentrates near the margin between teeth and gums, a pattern that is both aesthetically prominent and often confused with purely structural brasssmile. Good oral hygiene does not prevent all forms of brasssmile, but it meaningfully slows the progression of most of them.
⚗️ Cause 10: Whitening Product Overuse: The Counterproductive Cycle
In an era of readily available whitening products, a significant and underappreciated contributor to brasssmile is the misuse of those very products intended to treat it. Hydrogen peroxide and carbamide peroxide, the active whitening agents in commercial strips, gels, and trays, function by penetrating enamel and breaking down stain molecules through an oxidative process. Used correctly and within recommended frequency limits, they are safe and effective. Used excessively, they cause enamel dehydration, micro-fractures, and sensitivity.
Dehydrated enamel appears more opaque immediately after treatment, which creates a temporary brightening effect — but rehydration over the following 24 to 72 hours can reveal an underlying warmth that feels like a retrograde step to the user. This drives repeated application, creating a cycle of over-treatment. Some popular charcoal and abrasive whitening products compound the problem by physically scratching enamel surfaces, creating microscopic grooves in which future staining compounds settle more readily. The result is paradoxical: excessive whitening product use can accelerate the structural enamel damage that makes brasssmile worse over time.
Quick Reference: Brasssmile Causes, Mechanisms and Reversibility
▶ Surface-based causes such as coffee, tea, red wine, and poor hygiene are generally the most responsive to whitening treatment. Structural causes — ageing, genetics, fluorosis, and medication-related staining — are less responsive to peroxide whitening and more often require professional intervention such as veneers, bonding, or microabrasion for lasting results.
Table: Brasssmile Cause Summary
| Cause | Type | Reversibility with Whitening | Best Treatment Approach |
| Coffee & Tea | Extrinsic | High | Peroxide strips + rinsing habits |
| Red Wine | Extrinsic | High | Whitening + dietary adjustment |
| Tobacco | Extrinsic + Intrinsic | Moderate | Professional whitening or veneers |
| Natural Ageing | Structural | Low | Veneers, bonding, or professional trays |
| Genetics | Structural | Low | Veneers or composite bonding |
| Medications | Intrinsic | Low to None | Veneers or porcelain options |
| Fluorosis | Structural | Low | Microabrasion, bonding, or veneers |
| Acidic Diet | Structural (erosion) | Moderate | Enamel protection + whitening |
| Poor Hygiene | Extrinsic | High | Scale & polish + improved routine |
| Whitening Overuse | Structural (dehydration) | Moderate | Rest period + remineralisation |
Common Mistakes People Make When Identifying Brasssmile Causes
▶ The most frequent mistake people make is assuming brasssmile has a single cause and applying a single treatment. Because most cases involve two or more causes operating simultaneously — for example, dietary staining compounding age-related enamel thinning — single-solution approaches consistently underperform. Accurate cause identification leads to layered, effective treatment strategies.
After years of seeing people try and abandon various whitening approaches, certain patterns emerge. The most consistent error is the assumption that brasssmile is purely a hygiene problem. It is not — and treating it as one leads to frustration. Over-brushing in response to a brassy smile can actually worsen enamel erosion, accelerating the structural component of the condition.
A second common mistake is choosing a whitening product based on marketing rather than mechanism. Charcoal toothpastes are frequently marketed as natural whitening solutions, but the clinical evidence for their effectiveness is weak and the evidence for their abrasive damage to enamel is growing. Someone with genetics-driven or age-related brasssmile who invests months in charcoal toothpaste is unlikely to see meaningful improvement — and may be causing incremental enamel damage in the process.
A third mistake is assuming that because whitening worked temporarily, the underlying cause has been addressed. Whitening removes staining but does not treat the causes that produced it. Without also addressing dietary habits, rinsing practices, or enamel remineralisation, the staining returns — sometimes within weeks — and the cycle restarts. Treating cause and symptom together is the only approach that produces genuinely lasting results.
⚠️ Never increase whitening product frequency in response to disappointing results. More product, used more often, compounds enamel dehydration and can worsen the structural dimensions of brasssmile over time. If standard whitening is not delivering lasting results after four to six weeks of correct use, the cause is likely structural and professional consultation is the appropriate next step.
Brasssmile Causes — Frequently Asked Questions
▶ These FAQs cover the most commonly searched questions about what causes brasssmile. Each answer is structured for clarity and directly addresses the specific concern behind the question.
Can brasssmile be caused by one thing alone?
In most cases, no. A brasssmile develops through the combined effect of multiple factors — dietary habits, enamel thinning, genetics, and sometimes medication history — working together over months or years. Occasionally, a single dominant cause is identifiable (such as tetracycline-related intrinsic staining), but even then, other contributing factors usually compound the effect. Treating multiple causes simultaneously produces better outcomes than targeting any single one.
Is brasssmile a sign of poor oral hygiene?
Not necessarily, and this is one of the most important misconceptions to correct. Many people with meticulous oral hygiene develop brasssmile due to natural ageing, genetic factors, or dietary habits. Equally, poor hygiene can be a contributing factor — but it is rarely the sole cause. Brasssmile is a multi-factorial cosmetic dental condition, not a measure of how carefully someone cleans their teeth.
Does coffee always cause brasssmile?
Coffee is a consistent contributor to surface staining that can develop into brasssmile over time, but it does not produce brasssmile in isolation for everyone. The impact of coffee depends on frequency of consumption, how long it remains in contact with teeth, whether the person rinses with water afterwards, and the baseline condition of their enamel. Someone with naturally thick, well-mineralised enamel who rinses consistently may drink coffee daily for years with minimal visible impact. Someone with thin enamel or a dry mouth — which reduces protective saliva — may see staining develop more quickly.
Can you inherit brasssmile from your parents?
Yes, partially. The thickness and natural shade of your tooth enamel, as well as the inherent colour of your dentin, are heritable traits. If both parents have always had a noticeably warm or brassy smile despite good oral health practices, there is a meaningful genetic component to your own risk. This does not mean the condition is unavoidable or untreatable, but it does mean that home whitening alone may have limited effectiveness and that professional cosmetic options may be worth exploring earlier than they might be for someone without a genetic predisposition.
Why do my teeth look brassy near the gumline specifically?
Brasssmile that concentrates near the gumline is usually caused by one of two things: either tartar (calcified plaque) accumulation in that zone, which is the first area plaque deposits and the hardest area to clean thoroughly with a standard toothbrush, or gum recession that exposes the more yellow root dentin, which lacks the enamel covering that the crown of the tooth has. Both require different interventions — the former responds to a professional scale and polish; the latter may require assessment by a dental hygienist or dentist.
Experience Perspective: What Dealing With Brasssmile Actually Feels Like
▶ For many people, recognising brasssmile is a gradual and sometimes emotionally charged process. Understanding it through lived experience — noticing it in photographs, feeling self-conscious in bright lighting, or realising that whitening products are not working as expected — is part of what makes finding reliable, cause-specific information so valuable.
There is a very specific moment many people describe when talking about noticing their brasssmile for the first time. It is not usually in a dentist’s chair or in front of a mirror. It is most often in a photograph — a wedding, a professional headshot, a candid snapshot taken in natural daylight — where the camera captures something the bathroom mirror at 7am somehow never quite shows. That warm, golden tint. The slight dullness. The sense that the smile looks a little off even though you cannot immediately say why.
What follows for many people is a period of trying every whitening product available — strips, serums, special toothpastes, oil pulling, charcoal powders — with varying degrees of success and a recurring sense that improvements are temporary at best. This is often because the products are being used without knowledge of the underlying cause. A whitening strip used on teeth where the brasssmile is primarily driven by thinning enamel and exposed dentin will produce a brief surface improvement that fades within days, leaving the person feeling like whitening simply does not work for them.
The shift that makes a genuine difference — both practically and psychologically — is understanding the cause. When you know whether your brasssmile is primarily extrinsic (surface staining from dietary and lifestyle factors) or structural (enamel thinning, dentin exposure, or intrinsic pigmentation), you stop reaching for products at random and start applying solutions with purpose. That purposeful approach is what BrassSmiles.org is built to support — and it is what makes this guide worth reading before you buy your next whitening product.
💡 The most valuable thing you can do before treating your brasssmile is to correctly identify its cause. Every decision that follows — which product to use, whether to visit a dentist, what dietary changes to prioritise — becomes more effective the moment you know what you are actually dealing with.
Next Steps: From Identifying the Cause to Choosing the Right Solution
▶ Once you have identified which of the 10 causes applies to your brasssmile — or which combination — the path to improvement becomes clear. Surface causes respond to peroxide-based whitening combined with dietary and rinsing habit changes. Structural causes respond best to professional treatments including custom trays, bonding, or veneers. Mixed cases benefit from a layered approach that addresses both dimensions.
Understanding your specific cause is not the end of the journey — it is the beginning of a smarter one. If your brasssmile is driven primarily by coffee and tea consumption, a combination of whitening strips, improved rinsing habits, and a blue-covarine toning toothpaste can produce real and lasting results. If it is driven by ageing and genetics, investing heavily in OTC whitening products will likely disappoint — but a conversation with a cosmetic dentist about veneers or professional bonding could genuinely transform your smile.
BrassSmiles.org covers every aspect of this journey — from cause identification through to solution selection, product comparison, and professional treatment guidance. Use the internal links throughout this guide to navigate to the articles that are most relevant to your specific situation. You now have the foundational knowledge. The practical steps are waiting for you.